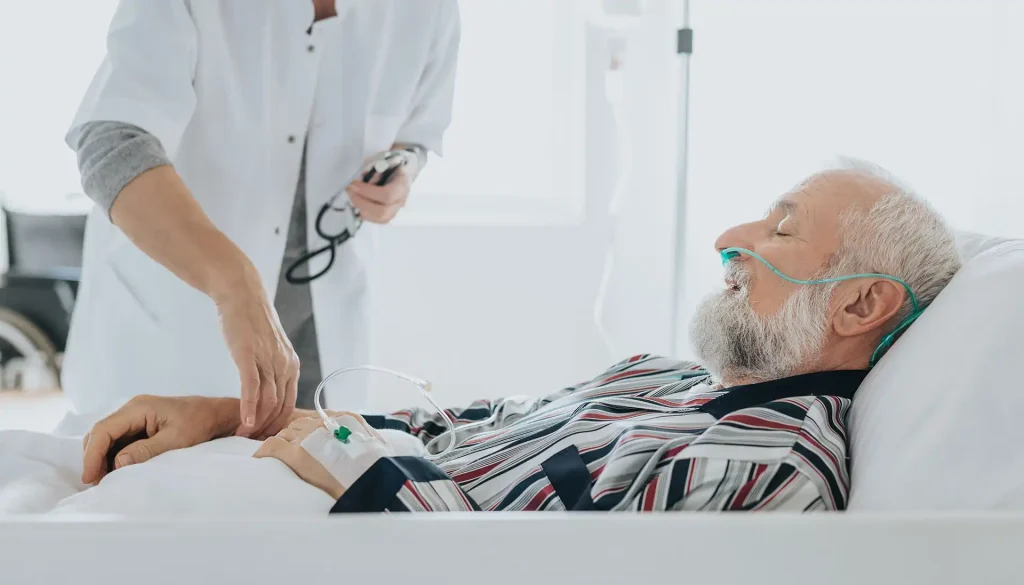
Cancer is one of the leading causes of illness worldwide, with around 20 million new diagnoses every year. Roughly half of people with cancer experience pain linked to the disease itself or to its treatment.
A recently published study in Progress in Palliative Care has evaluated two-year longitudinal data from UK adults prescribed cannabis-based medicinal products (CBMPs) for cancer-related pain following inadequate symptom control from conventional therapies. This analysis investigates the study’s parameters, temporal changes in patient-reported outcomes, and, crucially, the inherent limitations that contextualise these findings.
What is cancer-related pain, and why is new research needed?
Cancer pain has many causes. It may come from pressure on tissues or nerves, from inflammation, or from the effects of surgery, chemotherapy or radiotherapy. Because of this, most patients need a combination of approaches to manage pain well.
Strong pain medicines known as opioids remain a core part of cancer pain management and work well for many people. However, around 1 in 4 patients still report that their pain is not well enough controlled on opioids alone, and some experience side effects that are hard to tolerate. Because people with cancer are living longer than in the past, the long-term effects of pain medicines are also an increasingly important consideration.
These unmet needs have led researchers to look at other options, including medical cannabis. In the UK, medical cannabis may be considered by a specialist only after licensed treatments have been tried and have not provided enough benefit.
What is the UK Medical Cannabis Registry?
The UK Medical Cannabis Registry (UKMCR) was set up by Curaleaf Clinic in 2019. It collects real-world information from patients across the UK who have been prescribed cannabis-based medicinal products for a range of conditions. The aim is to build a clearer long-term picture of how symptoms change and what side effects are reported.
The research discussed here was carried out by a team that includes Curaleaf Clinic staff.
What did the study look at?
The research team looked at 116 adults whose main reason for treatment was cancer-related pain, and who had been enrolled in the registry for at least two years. Each patient had previously tried licensed pain treatments and continued to experience pain that was not well enough controlled.
Of the patients included, most had advanced disease. Around 61% had cancer that had spread beyond its original site, around 33% had localised disease, and 6% no longer had a solid tumour at the time they joined the study. The average age was 56 years, and a little over half of the participants were employed at enrolment.
Patients completed a set of questionnaires before starting treatment (baseline) and then at 1, 3, 6, 12, 18 and 24 months. Any side effects were recorded throughout.
Which questionnaires were used?
The researchers used a mix of pain-specific and general health questionnaires:
- Pain Visual Analogue Scale (Pain VAS) — a simple 0–10 rating of current pain intensity.
- Brief Pain Inventory — Short Form (BPI) — covering both pain severity and how pain interferes with daily life.
- EQ-5D-5L — a widely used measure of health-related quality of life, covering mobility, self-care, usual activities, pain/discomfort and anxiety/depression.
- Generalised Anxiety Disorder-7 (GAD-7) — a measure of anxiety symptoms.Single Item Sleep Quality Scale (SQS) — a simple rating of sleep quality.
- Patient Global Impression of Change (PGIC) — the patient’s own view of how much their condition has changed since starting treatment.
What did the findings show?
The study reported changes in average scores across the group. None of these results mean a medicine worked for any one person — they are group-level observations without a comparison group.
Did pain scores change?
Average BPI Severity scores were lower than baseline at every time point from 6 months onwards, with the biggest average change seen at 18 months. Average BPI Interference (how much pain gets in the way of daily life) was lower at some time points but not all. Pain VAS was lower at 6 months, though changes at other time points did not reach statistical significance.
At 24 months, meaningful change thresholds were reached by around 50% of patients on the Pain VAS, around 47% on BPI Severity, and around 54% on BPI Interference.
What about quality of life, anxiety and sleep?
Average EQ-5D-5L index scores increased from 0.38 at baseline to 0.62 at 24 months, suggesting a change in overall perceived quality of life at the group level. Average anxiety scores (GAD-7) and sleep quality scores (SQS) also improved compared with baseline across most follow-up points. Mobility and self-care domains, however, did not change significantly.
What do these numbers actually mean?
A change in an average group score is not the same as a treatment “working.” Some patients will improve, some will stay the same, and some will get worse. In cancer pain specifically, scores can also change because the underlying disease changes, because other treatments are added or adjusted, or because of natural variation over time. Without a control group, it is not possible to separate these effects from any effect of the medicine.
What side effects were reported?
Five of the 116 patients (4.31%) reported a total of 55 side effects over two years. Of these, 45.45% were classed as mild, 32.73% as moderate and 21.83% as severe. No life-threatening or fatal side effects were recorded.
The most commonly reported side effects were fatigue, lethargy, impaired concentration, nausea and constipation. Notably, every patient who reported a side effect had not used cannabis before starting treatment. The authors suggest this may point to a need for more cautious dose titration and more intensive monitoring for people who are new to cannabis.
How should these findings be interpreted?
The authors are clear that this type of study cannot prove that medical cannabis caused any of the changes reported. Several factors make interpretation particularly difficult in cancer populations:
- No control group or blinding. Without a comparison group, improvements could reflect placebo effect, the natural course of the disease, regression to the mean, or changes in other treatments.
- Disease progression and survivorship. Patients who did worse, became more unwell or died were less likely to complete later questionnaires. This means the group still responding at 24 months may have had a more favourable disease course than the group as a whole.
- Changes to other treatments. Cancer care often changes over time. The study did not control for adjustments to other pain medicines, anticancer treatments or supportive care, all of which can influence symptoms.
- Self-reported outcomes. Scores come from patient questionnaires, which can be influenced by expectation, memory, fatigue and mood. In cancer, distress and pain catastrophising can also inflate baseline scores.
- Possible differences between cancer and non-cancer pain. Recent reviews suggest medical cannabis may have a smaller effect on cancer-related pain than on some non-cancer chronic pain conditions. Evidence from other pain populations should not be assumed to apply to cancer pain.
- Unknown treatment-related attribution. Side effects in this study were not formally assessed for whether they were caused by the treatment, so cannot be directly attributed to it.
What does this mean for people living with cancer pain in the UK?
Cancer pain management in the UK is led by oncology, palliative care and specialist pain teams, supported by GPs. It usually combines several approaches, including non-opioid pain medicines, opioids when appropriate, nerve pain medicines, interventional techniques such as nerve blocks, radiotherapy for pain, physiotherapy, and psychological support. Hospice and community palliative care services play an important role.
Medical cannabis is not a first-line option for cancer pain. National UK guidance does not routinely recommend it for this indication, and the most recent reviews have not shown consistent benefit in cancer pain specifically. In practice, it may be considered by a specialist only when licensed treatments have been tried and have not provided enough benefit, and when an individual assessment supports it.
Research like the study described here adds to the limited evidence base but does not change standard clinical practice. Larger, better-controlled trials, including randomised controlled trials, are needed before firm conclusions can be drawn.